Researchers from the Department of Molecular Biology and Genetics at Koc University in Turkey and the Pole of Endocrinology, Diabetology and Nutrition, Institute of Experimental and Clinical Research at Université Catholique de Louvain in Belgium, have collaborated to interrogate the mechanisms behind a cancer-associated wasting syndrome—cachexia.
The paper “EDA2R–NIK signalling promotes muscle atrophy linked to cancer cachexia,” published in Nature, details the discovery of how an alternative splicing of ectodysplasin A (EDA) leads to a signaling pathway in cachexia pathology. A News & Views piece published in the same journal outlines the study’s findings.
EDA, a type of cytokine, belongs to the tumor necrosis factor (TNF) superfamily of signaling proteins made by white blood cells to do the work of the immune system. Researchers discovered that an alternative splicing of EDA, EDA2R messenger RNA, was enriched in the skeletal muscle tissues of mice with the wasting syndrome cachexia.
Wasting syndrome
Cachexia most often appears in advanced pancreatic and lung cancer and frequently with colorectal, ovarian, and liver cancers.
Defined as losing 5% or more of body weight over the preceding six months, cachexia can also induce fatigue and reduced strength. The definition alone is a crude measure of a more complex physiological condition that can be missed in diagnosis as it overlaps similar effects that cancer treatments can have.
Physical atrophy with cachexia can accelerate as the patient may be unable to perform routine tasks like bathing, shopping or feeding themselves, either from a lack of physical energy or absence of appetite. Mental health issues can quickly follow. Additionally, the fallout from cachexia is considered to be directly causal to nearly a third of cancer deaths when heart or respiratory failure due to muscle loss occurs.
Without a known mechanism, even a diagnosis can have limited use in clinical settings without effective treatments and a clear course of action.
Intriguing correlation
Through gene expression searches in muscle biopsies, the researchers detected elevated EDA2R mRNA in patients with cachectic cancers (lung, gastrointestinal, pancreatic and colorectal cancers) when compared to cancer patients without cachexia and cancer-free controls.
Additionally, the team found that patients suffering from reduced muscle mass and function with Duchenne muscular dystrophy (DMD) and facioscapulohumeral muscular dystrophy (FSHD) also had significantly elevated EDA2R transcript.
With the EDA-A2—EDA2R pathway correlation detected, researchers pursued the investigation further.
Discovering mechanisms
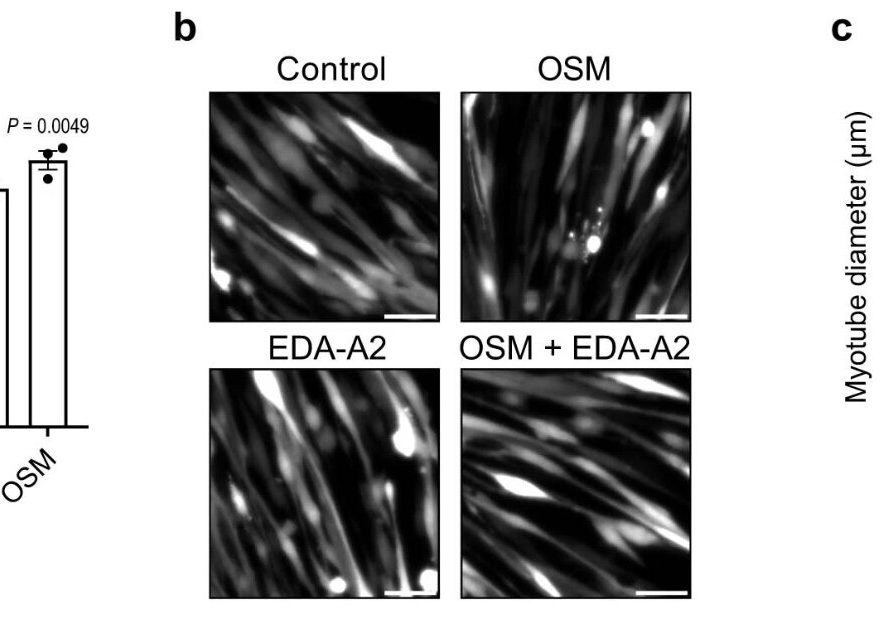
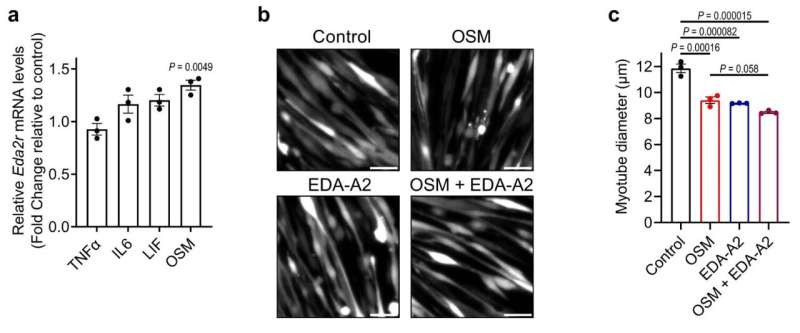
Starting with tissue cultures and advancing to a mouse model, the team repeatedly found that enhanced EDA-A2 protein levels had deleterious effects. They observed a cell size reduction in the tissue cultures, and in vivo mice experiments showed profound muscle degeneration.
The experiments also revealed downstream effects of EDA-A2 after interacting with its receptor. NFĸB-inducing kinase (NIK), a key regulator of transcription factors that control the expression of a significant number of genes, is set in motion to activate genes that transcribe enzymes that can break down muscle tissues.
Upstream of the receptor EDA2R expression, researchers identified tumor-induced oncostatin M (OSM) as a key up regulator. Depletion of OSM messenger RNA in muscles protected them against wasting and atrophy.
The study results suggest that OSM–OSMR signaling acts in parallel with the EDA2R–NIK pathway and reinforces muscle atrophy and EDA2R upregulation.
Deleting either EDA2R or NIK in mice was sufficient to confer resistance against tumor-induced muscle wasting. The authors suggest targeting the OSM–OSMR pathway could also be a high-value therapeutic target.
As with the end of any good study, more research is needed. The next steps may be determining which targets hold the best risk-benefit ratios and advancing the understanding of causal relationships toward a clinical intervention.
More information:
Sevval Nur Bilgic et al, EDA2R–NIK signalling promotes muscle atrophy linked to cancer cachexia, Nature (2023). DOI: 10.1038/s41586-023-06047-y
Laura Antonio-Herrera et al, Molecular basis for muscle loss that causes cachexia, Nature (2023). DOI: 10.1038/d41586-023-01527-7
Journal information:
Nature
Source: Read Full Article